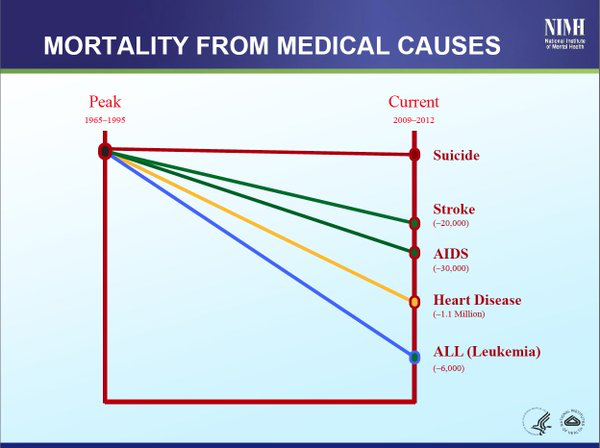
September is Suicide Prevention Month and well-meaning suicide advocates are out in force calling for a greater effort to reduce it. But can we reduce suicide? While researching, “Insane Consequences: How the Mental Health Industry Fails the Mentally Ill,” I learned that mortality from strokes, AIDS, heart disease, and leukemia have decreased dramatically since the 1960s, but in spite of all we’ve spent on suicide, suicide mortality has remained the same.
Suicide is always devastating to the affected families and communities, but it is relatively rare which makes it difficult to predict and research. 44,000 suicides were completed in 2015, representing just .013 percent of the population.
“Suicide is always devastating to the affected families and communities, but it is relatively rare which makes it difficult to predict and research.”
One strategy promoted by suicide prevention advocates to reduce suicide is to raise awareness. But a large analysis of the literature published in the Journal of the American Medical Association, found, “Public education and awareness campaigns, largely about depression, have no detectable effect on primary outcomes of decreasing suicidal acts.”
Another strategy embraced by the suicide advocates is to target prevention efforts at youth (suicide is the second leading cause of death in those under 24). But that’s only because people in that age group rarely die of anything. They are the least likely to take their own lives. According the American Foundation for Suicide Prevention, “In 2015, the highest suicide rate was among adults between 45 and 64 years of age. The second highest rate occurred in those 85 years or older.” Suicide is mainly an adult event. “Younger groups have had consistently lower suicide rates than middle-aged and older adults.”

As a result of work by the child-lobby, in 2016, Congress targeted $54 million in suicide prevention funds to the under 24 group and only $2 million to address the larger and older group. Much of the suicide effort takes place on college campuses, but college students are less likely than same-aged non-college students to have serious thoughts of suicide.
And is “serious thoughts of suicide” the most important metric? Almost all programs that claim success at reducing suicide attribute their success to proxy or association measures, rather than the number of suicides. Programs will label themselves a success based on the number of calls to a hotline, a measurable change in attitude among a sample population, self-reports of help-seeking behavior and numerous other metrics except for the one that counts the most: the number of suicides.
There may be effective ways to reduce suicide, but they are not the ones most advocates focus on and they need more research. One of the highest concentrations of suicide is in prisoners. Those suicides are perhaps the easiest to prevent because corrections officials control the environment and have the ability to remove the means used to effect suicide.
Means removal may also be effective for the non-incarcerated. Depending on who you believe, between 6,000 and 20,000 people with mental illness killed themselves with a gun in 2015, so installing locks on guns or preventing high-risk groups like the mentally ill and previous suicide attempters from buying guns might be effective suicide prevention tools. But because suicide is so rare, most of the guns with locks and people prevented from buying guns would not be people who want to commit suicide.
About 13 percent, or about 5,000 suicides, are likely committed by people with a serious mental illness. The lifetime risk to those with schizophrenia is 5 percentand to those with bipolar disorder is 10 -15 percent. Suicide rates are up to 15 times higher for people with serious mental illness in the 90 days following discharge from a psychiatric hospitalization. So keeping the seriously mentally ill in treatment might help reduce suicide, even if it has to be involuntary treatment. One study found the “consequences of treatment nonadherence [to antipsychotics] include a fourfold increase in the risk of suicide.” There is evidence clozaril, lithium, and possibly electroconvulsive therapy decrease the incidence of suicide among individuals with severe psychiatric disorders.
We do know that suicide is rare and we haven’t reduced it. So maybe it is time to do more research of higher quality rather than continuing with the mass implementation of what doesn’t work.
This piece originally appeared at RealClearHealth
______________________
DJ Jaffe is Executive Director of Mental Illness Policy Org., and author of Insane Consequences: How the Mental Health Industry Fails the Mentally Ill.
This piece originally appeared in RealClearHealth
